Pre op Packet Motion Academy
The Motion Academy
Your Educational Guide to Total Joint Replacement
Michael J. Sumko, DO
Drew Lambourne, PA-C
_______________________________
Medical Assistants – Kimberly and Angela
480-558-3744 (ext. 7517)
Surgery Scheduler – Belinda
(belinda.lujan@tenethealth.com)

The goal of our team is to alleviate joint pain and restore function, returning you to desired activity. To meet this goal, we partner with you to provide an optimal outcome through education, preparation, nutrition, rehabilitation, and minimal invasive surgical technique.
We thank you for your trust and confidence.
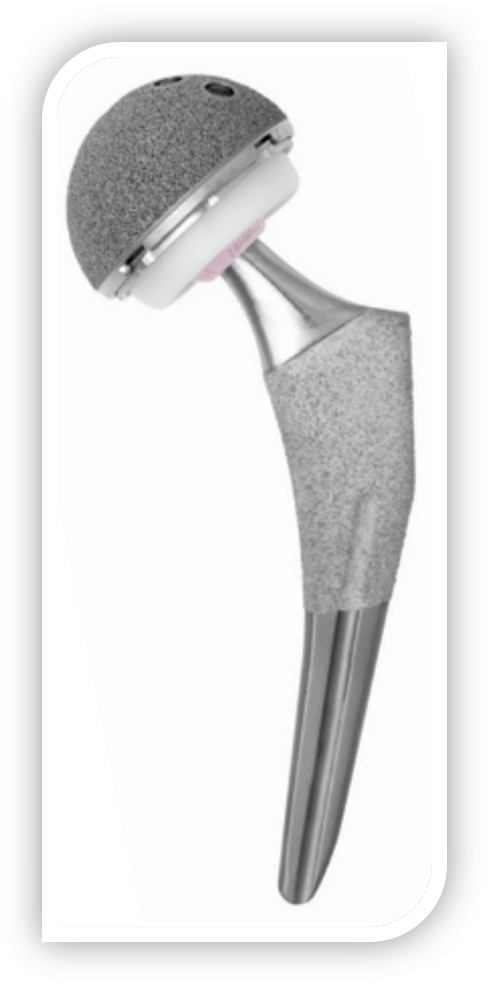
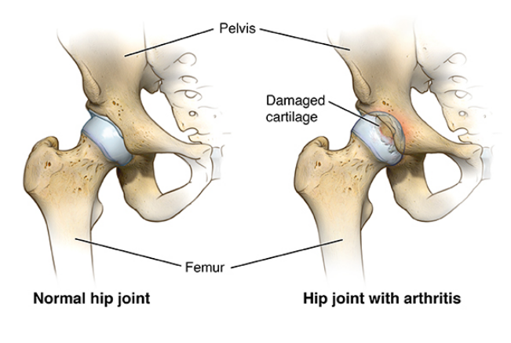
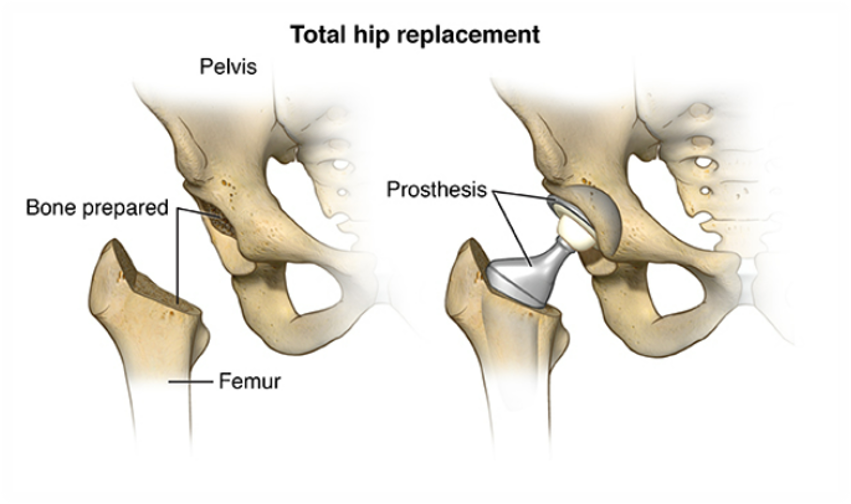
Understanding Hip & Knee Replacements

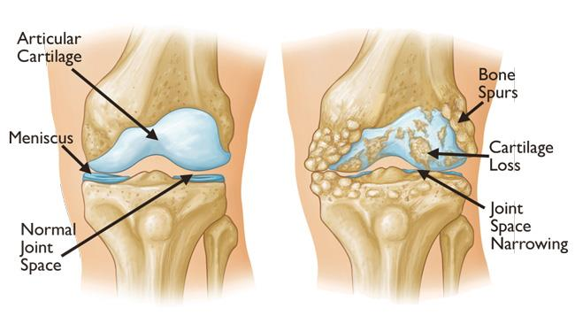
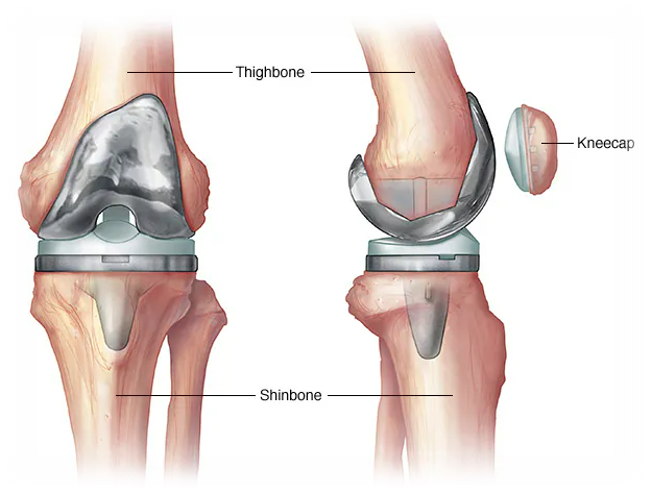
AVOID COMPLICATIONS BY REDUCING RISKS

2. STOP SMOKING/NICOTINE: 3 MONTHS BEFORE & 3 MONTHS AFTER
3. STOP ALL SUPPLEMENTS AND VITAMINS: 3 WEEKS BEFORE SURGERY
4. CONTROL BLOOD SUGARS: KEEP HEMOGLOBIN A1C LESS THAN 7.0

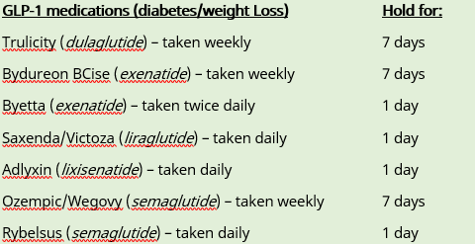
MEDICATIONS TO STOP
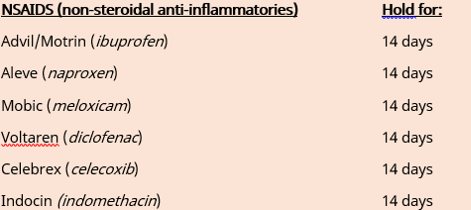





Your journey to a faster recovery
Preserve Muscle Mass
Promote Wound Healing
Support bone health
Enhance Immune Function


- PROTEIN ISOLATE
- CREATINE
- CALCIUM
- VITAMIN D
Nutrition Matters
Tried. Trusted. Recommended.

Before Surgery
- DO NOT EAT OR DRINK ANYTHING AFTER MIDIGHT (except for medications instructed by your surgical team\Weight
- Shower with Hibiclens soap 24 hours before
- Do not shave the area of your surgery for 3 days prior
- Increase water intake for the day before surgery
- Prepare what to bring to the hospital
- Bring picture ID and insurance cards


Day of Surgery (Pre-Op)
- Do not wear makeup, lipstick, or Jewelery to the hospital
- Arrive at the hospital 2 hours prior to your scheduled surgery time
- Go to the Admitting Department to register
- You and your family member or caregiver will be accompanied from the Admitting Department to the Pre-Op area after you have been registered
- Your Pre-Op nurse will have you changed into a hospital gown, take your vital signs, review your personal history and review your medication reconciliation form. You will be administered an IV
- Sign the surgical and blood consent forms
- Meet with the anesthesiologist, who will discuss the plan for anesthesia. Sign the anesthesia consent form.
- Meet your surgical nurse
- Meet with your surgeon, who will mark the correct surgical site with a black marker pen.
- You will receive an antibiotic through your IV prior to your surgery and you may receive pre-anesthesia medication
- You are now ready for the operating room. The surgeon will speak with your family member after your surgery is completed.
After Surgery (PACU)
- Your vital signs will be monitored frequently, until stable.
- You will be placed in a hospital bed.
- You will have a dressing on your surgical wound.
- Your surgeon may order an X-ray to be taken of your surgical area.
- Your nurse will assess your pain level and provide medications through your IV, as needed.
- Once you are awake enough and do not feel nauseated, you will be allowed ice chips and liquids.
- You will have an icepack on the surgical area.
- You will have compression stockings on both legs to prevent deep vein thrombosis (DVT) (blood clots in the legs).
- If you are going home the same day as surgery, the Physical Therapist will see you in the recovery bay, and will instruct and assist in simple exercises to help you understand your limits and keep you safe.
Immediate Post-Op Physical Therapy
The physical therapist or recovery nurse will see you shortly after your surgery once you are alert and stable. Initially, they will instruct you on:
- How to get in and out of bed safely.
- Transferring from seated to standing positions.
- Proper ambulation sequence with the walker:
- Place walker forward, at arms length. Stand up, don’t hunch over.
- Step forward with operative leg.
- Step forward with non-operative leg.
- Your weight bearing status will be Weight Bearing as Tolerated, unless instructed otherwise by Dr. Sumko.
- Exercises to improve your strength, mobility, and increase your endurance.
- Any restrictions, if necessary.
Discharge Home
OUTPATIENT SURGERY – In most cases, you will be discharged on the same day as your surgery from the hospital/surgery center to your home. The goal is to get you back home.
Once you have completed your session of physical therapy, your vitals are stable, and you are found to be medically stable, you will then be discharged home.
Before leaving the hospital or surgery center, make sure your questions and all other concerns have been answered and addressed.
To facilitate the best and quickest recovery, and to promote optimal function of your new joint, you must continue exercising and adhering to any restrictions given to you when you return home.
Pain Management
Day of Surgery
- The anesthesia provider will perform a spinal block
This will “numb” the pain in operative leg, which will decrease the amount of drugs that will be required during surgery. This will allow you to wake up and be more alert quickly after surgery with less side effects.
- A nerve block will be performed on patients receiving a total knee replacement.
This nerve block typically lasts between 24 and 48 hours. During this time, you may experience some tingling or numbness in the affected extremity, all of which return to normal once the nerve block wears off.
After Surgery
- Apply ice machine/cold to the surgery site 30 minutes of every hour with foot elevated above your knee.
- brace ice recovery unit, can be set for 30 on 30 off and remain on overnight while you sleep.
- When not icing and elevating leg, remove Nice Machine brace and do gentle range of motion or Rom Bike.
- Follow the instructions in regards to post-operative pain meds.
- You may experience varying degrees of discomfort. This is normal and will improve with each day.
- The goal of pain management is to maintain a level of comfort enables you to participate in activities and rest.
- Pain control is essential to your recovery and will improve your ability to eat, sleep and exercise.
4 Post-Operative Medications you will be prescribed and required to take:
1.Baby Aspirin 81 mg (Blood Thinner)
1.One pill twice a daily for 6 weeks. Begin the morning after surgery.
2.If you are already on a blood thinner (Lovenox, Coumadin, Plavix, Xarelto, Eliquis, etc.) – then you DO NOT take the baby Aspirin, and RESUME your regular blood thinner the day after surgery.
2.Meloxicam 15 mg (Anti-inflammatory)
1.One pill, daily, in the morning with food and water for 4-6 weeks for swelling
2.DO NOT TAKE:
a.If you have an allergy to NSAIDs (i.e. ibuprofen, naproxen).
b.History of stomach or kidney problems.
c.Have cardiac stents
d.Currently on a prescription blood thinner.
3.Acetaminophen 500 mg (Pain medication) THIS is your primary pain medication.
1.Two pills every 6 hours until you no longer have pain.
2.Don’t take more than 4000mg in a 24 hour period.
4.Cephalexin 500mg (Antibiotic)
1.Take one pill 3 times a day for 5 days. Begin at 8pm on day of surgery
4 Post-Operative Medications you will be prescribed and required to take
1.Oxycodone 5 mg (Narcotic pain pill)
1.One pill every 6 hours as needed for breakthrough pain. This means that if your Tylenol isn’t providing 6 hours of relief, then you can take a 5 mg oxycodone pill in between your Tylenol pills. Get off the Oxy as soon as you can make it 6 hours with just Tylenol.
2.You will only be given 30 pills, so use them wisely. Ice and elevation will be your friend. These pills cause constipation, nausea, and other side effects.
3.Most patients only take Oxy before or after therapy and at night to help them sleep for the first few days.
2.Cyclobenzaprine 10 mg (Muscle relaxer)
1.Only take every 8 hours as needed for spasms.
2.Some will take at night to help with sleep. A common side effect is drowsiness.
3.Do not plan on leaving the house if you take one.
**Over-the-counter Benadryl (25-50mg) every 4 hours and/or Melatonin is oftenrecommended as a sleeping aid.
Blood Clot Prevention
Preventing deep vein thrombosis (DVT or blood clots in legs) is a priority after joint replacement surgery.
Anticoagulant (Blood Thinner)
- Dr. Sumko will prescribe Aspirin 81mg twice a day to help with blood thinning.
- If you have a history of blood clots, you will be prescribed a different blood thinner.
- If you are currently taking an anticoagulant, then you will resume that medication the following day after surgery.
- If your insurance approved the post operative kit, you will were the calve compression devices or SCD’s 8 hours a day.
Your care team will be very focused on improving circulation in your lower extremities. You also need to take an active role in preventing this complication. If at any time you experience pain in your calves, please report it to your care team.
Blood Clot Prevention
Compression Stockings
You will have compression stockings or “TED Hose” applied to your legs after surgery. These should be worn day and night for a total of 4 weeks on the surgical leg and 2 weeks on the nonsurgical side.
These may be removed for 60 minutes daily, to be washed, for showering, etc.
The TED Hose also serves well as a barrier between your skin and the ice wraps.
Do not allow the stockings to bunch up on your leg and form creases —
the stockings should be kept smooth.
https://youtu.be/q-i_TwaoPkY – watch for tips for application
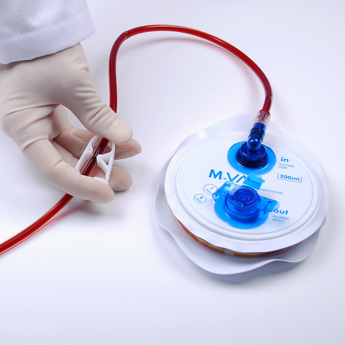
Drain – with Total Knee Replacement
During surgery, you likely will have a drain placed to draw any excess fluid from your surgical site.
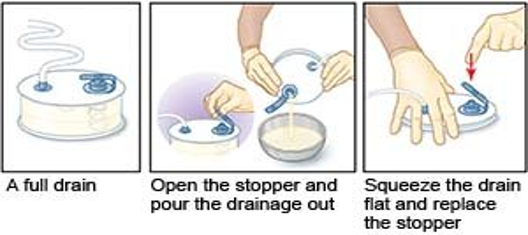
The day after surgery at 5:00pm, you will need to remove the drain by:
1.Unplug the stopper to undo the suction.
2.Remove the clear tape on the side of leg and gently pull out the tubing from the knee
3.Immediately place a gauze and compression over the drain site, followed by a Band-Aid or dressing.
Dressing/Incision Care
After your surgery, your incision will be covered with a large dressing for protection and to promote cleanliness. There may be some blood or fluid absorption on the dressing. If the dressing becomes saturated and thefluid leaks from the bandage, contact the office.
Keep bandages covered with shower bag, or glad press and seal while showering to keep dry.
Hips: You will be able to remove your dressing in 12 to 14 days on your own. You will have steri-strips under the dressing – keep them in place until they fall off on their own.
Knees: You may remove the Ace Bandage and padding when you return home and begin using the cold compression machine. Keep the TED hose stocking on.Use the Ace Bandage wrap if you leave your home. Your incision dressing will be removed at your post-op visit in 10 to 14 days
Post Operative Rehab Kit
If your insurance approves, OneSource Medical, LLC will order and deliver this rehab kit to your home or surgical center after surgery to help in your recovery.
This kit may include the following products:
1) ManaFlexx – Muscle Stimulator [Use 3 times a day]
2) Plasma Flow – Blood clot prevention [Use 8 hours a day]
https://youtu.be/8YyQhq8XMUQ?list=PLX6T1cBoLjCDuZksfHKJqNKwrIcHpLSR8
3) Cold Gel Pack Brace– Cold Therapy [After NICE machine rental, use 3-4 times a day]
https://youtu.be/0FwGyppzZVo (Knee)
Provided by OneSource Medical, LLC




- Covered by most major insurances, including Medicare.
- Delivered to your home, providing excellent in-home therapy for 3 weeks.
- Shown to improve range of motion and decrease overall pain.


*** To be used in addition to outpatient physical therapy ***
Provided by OneSource Medical, LLC if insurance approves


- Improve post-operative swelling and pain management.
- Reduce use of narcotic pain medications.
- Convenient, Consistent, Compression, Efficient.
- No hassle with re-freezing gel packs or ice bags.
- Only requires a cup of water to fill machine weekly.
- Provides Temperature Control and Compression Control.
- Program settings so you can set schedule and go to sleep. J
- Easy delivery and return of equipment.
- Available for 2 week rental or longer offered The Recovery Shop.

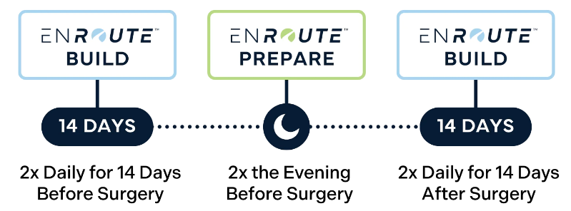
Used prior to Total Knee Replacement surgery
- Done 2 weeks prior to surgery
by Drew Lambourne, PA-C.
- Treatment effects last for 60-90 days
- Reduces narcotic pain med usage
- Avoid side effects from medications
- Improves physical therapy outcomes
- Cash Pay
Scan with your phone’s camera
to learn more.

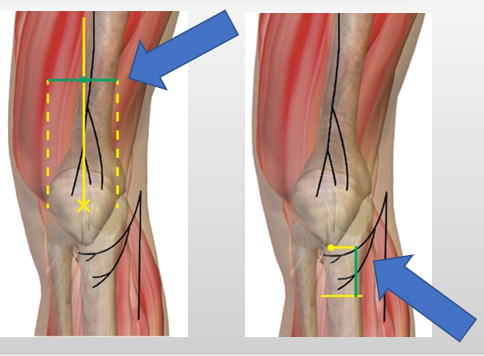
Cryoanalgesia of
superficial nerves of knee